2023 Scientific Meeting Poster Presentations with Abstracts
Reviewed & Presented by the AAOP Poster Committee
Poster 1
Insomnia is Associated with Higher Pain Intensity in Orofacial Pain Patients: A Cross- Sectional Study
Authors: Alessandri-Bonetti, A1,2; Sangalli, L3; Boggero, IA1,4
Affiliations: 1University of Kentucky, College of Dentistry, Department of Oral Health Science, Division of Orofacial Pain; Lexington, KY, USA. 2 Institute of Dental Clinic, A. Gemelli University Policlinic IRCCS, Catholic University of Sacred Heart; Rome – Italy. 3 College of Dental Medicine – Illinois, Midwestern University; Downers Grove, IL, USA. 4 University of Kentucky, Department of Psychology; Lexington, KY, USA
Poster 2
Nurses and Teachers are More Frequently Seen among Patients with Chronic Orofacial Pain. A Retrospective Study
Authors: Sangalli, L1; Alessandri-Bonetti, A2; Boggero, IA2,3
Affiliation: 1 College of Dental Medicine – Illinois, Midwestern University, Downers Grove, IL, USA. 2 Department of Oral Health Science, Division of Orofacial Pain, University of Kentucky, College of Dentistry, Lexington, KY, USA. 3 Department of Psychology, University of Kentucky, College of Arts and Science, Lexington, KY, USA
Poster 3
Are Educational Blogs a Suitable Strategy to Promote Awareness About Orofacial Pain- Related Topics? A 4-Year Outcome Report
Authors: Wang, JC; Botros, J; Padilla, M
Affiliations: Herman Ostrow School of Dentistry, University of Southern California, Los Angeles, CA
Poster 4
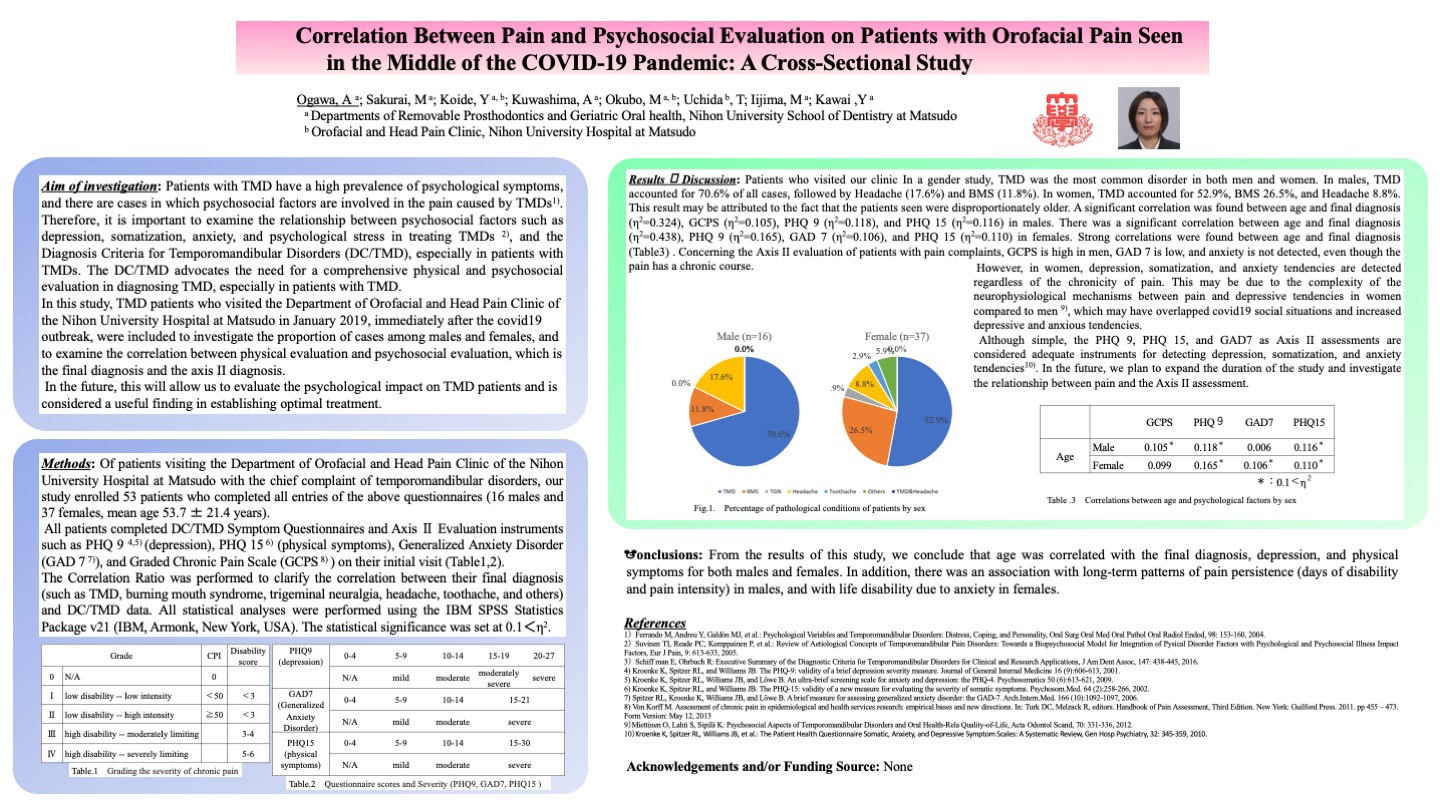
Correlation Between Pain and Psychosocial Evaluation on Patients with Orofacial Pain Seen in the Middle of the COVID-19 Pandemic: A Cross-Sectional Study
Authors: Ogawa, A; Sakurai, M; Koide, Y; Kuwashima, A; Okubo, M; Uchida, T; Iijima, M; Kawai,Y
Affiliations: Departments of Removable Prosthodontics and Geriatric Oral health, Nihon University School of Dentistry at Matsudo
Poster 5
Management of Concomitant Trigeminal Neuropathy and Myofascial Pain with Botulinum Toxin-A (BoNT-A)
Authors: Kandari, A; Sawani, S; Hernandez, I; Friesen, R
Affiliations: TMD/Orofacial Pain Clinic (Oral Medicine Graduate Program) University of Alberta, Canada
Poster 6
The DDS and ASPID Students’ Perspective Regarding the “Virtual Flipped Classroom, Case- Based” Pedagogy Introduced Through Orofacial Pain Module: A Quantitative Survey Study
Authors: Ahmadieh, A1 and Navazesh, M2
Affiliations: 1Clinical Assistant Professor, Herman Ostrow School of Dentistry of USC and Diplomate of American Board of Orofacial Pain. 2Professor and Associate Dean, Herman Ostrow School of Dentistry of USC
Poster 7
Agenesis of the Temporomandibular Condyle in a Three-Year-Old Patient: A Case Report
Authors: Benavides, S1 and Pérez, C2
Affiliations: 1Resident Orofacial Pain. University of Kentucky, Lexington. 2Associate Professor and Chief, Division of Pediatric Dentistry, University of Kentucky, Lexington
Poster 8
Myositis Ossificans of the Masseter Muscle – A Case Report
Authors: Alswaiti, O1 and Malacarne, A2
Affiliations: 1 Orofacial Pain Resident, Department of Diagnostic Sciences, School of Dental Medicine, Tufts University, USA. 2 Assistant Professor, Department of Diagnostic Sciences, School of Dental Medicine, Tufts University, USA
Poster 9
Clinical Reasoning Process in Patients with Temporomandibular-Related Somatic Tinnitus: A Case Series
Authors: van der Wal, AC 1,2,3; Visscher, CM 1; van der Meer, HA 1,3; De Hertogh, W2
Affiliations: 1 Department of Orofacial Pain and Disfunction, Academic Centre for Dentistry Amsterdam (ACTA), University of Amsterdam and Vrije Universiteit (VU) University Amsterdam, Amsterdam, the Netherlands. 2 Department of Rehabilitation Sciences and Physiotherapy, Faculty of Medicine and Health Sciences, University of Antwerp, Antwerp, Belgium. 3 SOMT University of Physiotherapy, Amersfoort, the Netherlands
Poster 10
Application of Bayesian Inference Algorithm in Orofacial Pain and Oral Medicine Diagnoses: A Retrospective Study
Authors: Vistoso Monreal, AP1; Veas, NA2; Loeb GE3; Clark, GT1
Affiliations: 1Herman Ostrow School of Dentistry, University of Southern California. 2McCombs School of Business, The University of Texas. 3Viterbi School of Engineering, University of Southern California
Poster 11
Inhibition of Nociception in a Preclinical Chronic TMD Model by Dietary Supplementation with Grape Seed Extract is Associated with Increased Expression of GABAergic Proteins in the Trigeminal Ganglion
Authors: Garten, DA; Antonopoulos, SR; Woodman, SE; Durham, PL
Affiliation: Missouri State University, Springfield, MO
Poster 13
Apnea-Hypopnea Index (AHI) and Oxygen Desaturation in Obstructive Sleep Apnea (OSA) Patients: A Retrospective Study
Authors: Masoudian Khouzani, M; Venturin, J; Sheppard, G; Sedghizadeh, P; Clark, G; Padilla, M
Affiliation: Orofacial Pain and Oral Medicine Clinic, University of Southern California
Poster 14
Squamous Cell Carcinoma Misdiagnosed and Treated as a Masticatory Muscle Disorder: A Case Report
Authors: Mishra, SS1; Guerrero, P2; Correa, L3
Affiliations: 1Resident, Department of Diagnostic Sciences, Tufts University School of Dental Medicine. 2Assistant Professor, Department of Diagnostic Sciences, Tufts University School of Dental Medicine.3Associate Professor, Department of Diagnostic Sciences, Tufts University School of Dental Medicine
Poster 15
Relationship between Migraine and Myofascial Orofacial Pain: A Systematic Review
Authors: Iturriaga, V1; Velásquez, N2; Bornhardt, C1; Thomas, DC4
Affiliations: 1Assistant Professor, Department of Integral Adult Care Dentistry, Temporomandibular Disorder and Orofacial Pain Program, Sleep & Pain Research Group, Faculty of Dentistry, Universidad de La Frontera, Temuco, Chile. 2Temporomandibular Disorder and Orofacial Pain Program, Faculty of Dentistry, Universidad de La Frontera, Temuco, Chile. 3Assistant Clinical Professor, Rutgers School of Dental Medicine, Newark, USA
Poster 16
Paradoxical Masseteric Bulging after Botulinum Neurotoxin Type A Injection: A Case Report
Authors: Sandhu, S and Shaefer, J
Affiliation: Mass General Hospital/Harvard School of Dental Medicine
Poster 17
HIV-Related Arthritis Affecting the Temporomandibular Joints: A Case Report
Authors: Taema, M1, 3; Uppgaard, R2; Herman, C1
Affiliations: 1 University of Minnesota Department of Diagnostic and Biological Sciences, Division of TMD and Orofacial Pain. 2 University of Minnesota Department of Developmental and Surgical Sciences, Division of Oral and Maxillofacial Surgery. 3 Cairo University, Department of Prosthodontics
Poster 18
Atypical Vestibular Migraine and Its Response to Various Treatment Modalities: A Case Report
Authors: Mehrotra, S and Eli, B
Affiliation: Private Practitioners
Poster 19
A Case Report on Post-Herpetic Neuralgia Treated with Infraorbital Nerve Blocks
Authors: Zaman, I and Handa, S
Affiliation: Massachusetts General Hospital/Harvard School of Dental Medicine
Poster 20
Parotid Gland Pain Presenting as Initial Symptom of Diabetes Mellitus: A Case Report
Authors: Koide, Y; Kuwashima, A; Ogawa, A; Sakurai, M; Okubo, M; Iijima, M; Uchida, T; Kawai, Y
Affiliation: Orofacial and Head Pain Clinic and Department of Removable Prosthodontics, Nihon University School of Dentistry at Matsudo
Poster 21
Metro vs Rural Orofacial Pain Patients: How Are They the Same, How Are They Different? A Retrospective Study
Authors: Dowling, MC1; Yanez-Regonesi, F1; Boggero, IA1,2,3
Affiliation: 1Department of Oral Health Science, Division of Orofacial Pain, University of Kentucky College of Dentistry, Lexington, Kentucky, USA. 2Department of Psychology, University of Kentucky College of Arts and Science, Lexington, Kentucky, USA. 3Department of Anesthesia, University of Kentucky College of Medicine, Lexington, Kentucky, USA
Poster 22
Neuromuscular Electrical Stimulation with Dry Needling Improved Muscle Function in Chronic Bell’s Palsy: A Case Report
Author: Blanchard, E and MacPherson, KL
Affiliation: Private Practitioners
Poster 23
Changes in Hearing Threshold and Auditory Brainstem Pathway Correlate with Trigeminal Nociception in a Preclinical Chronic TMD Model
Authors: Masten, A; Woodman, SE; Kaf, W; Durham, PL
Affiliation: Missouri State University, Springfield, MO
Poster 24
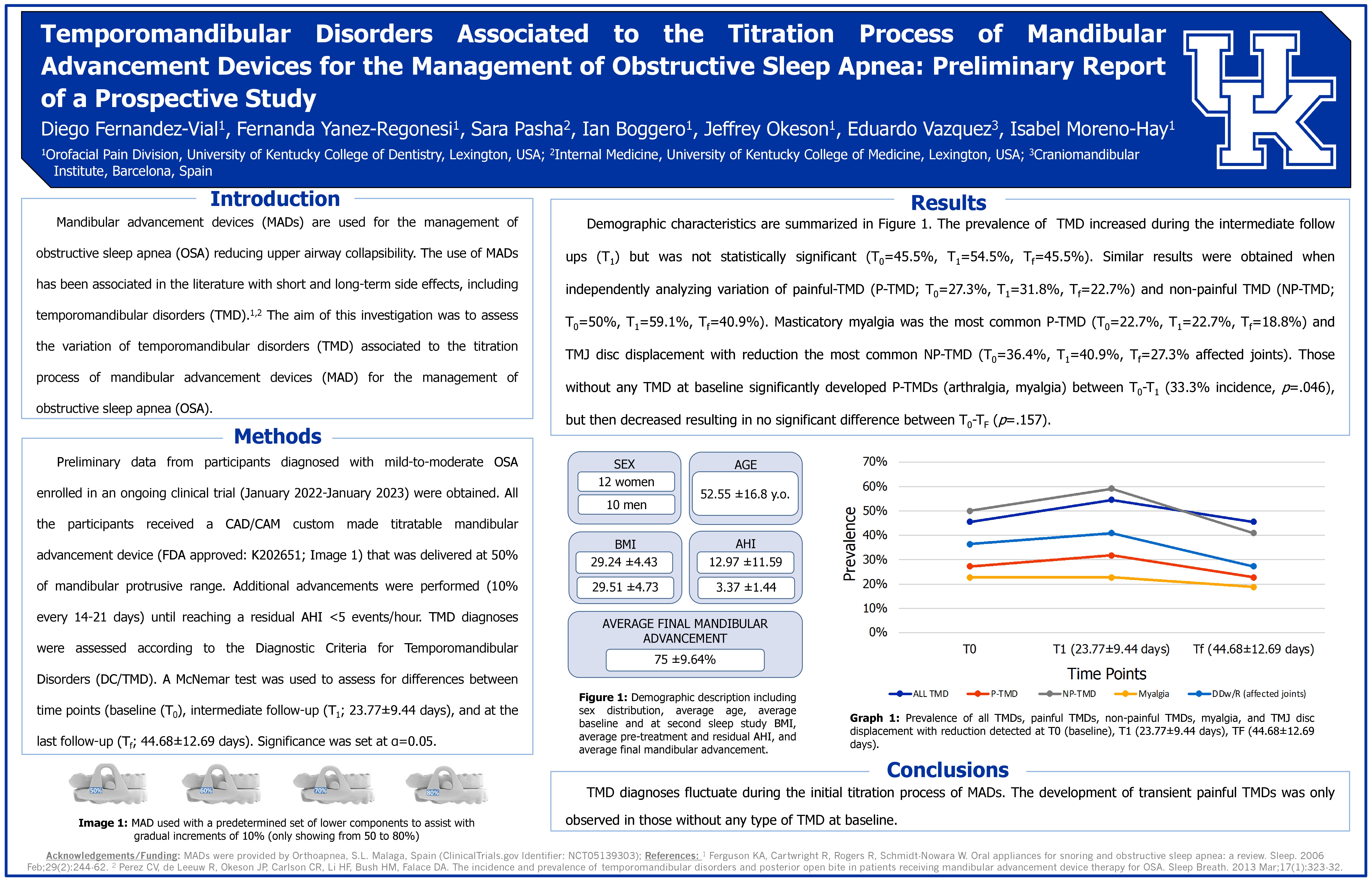
Temporomandibular Disorders Associated to the Titration Process of Mandibular Advancement Devices for the Management of Obstructive Sleep Apnea: Preliminary Report of a Prospective Study
Authors: Fernandez-Vial, D1; Yanez-Regonesi, F1; Pasha, S2; Boggero, I1; Okeson, J1; Vazquez, E3; Moreno-Hay, I1
Affiliations: 1Orofacial Pain Center, University of Kentucky College of Dentistry, Lexington, USA. 2Internal Medicine, University of Kentucky College of Medicine, Lexington, USA. 3Craniomandibular Institute, Barcelona, Spain
Poster 25
Perceived Origin of Pain as a Predictor of Pain Severity and Pain Descriptors: A Retrospective Study
Authors: Mitchell, A1 and Boggero, I1,2, 3
Affiliations: 1Department of Oral Health Science, Division of Orofacial Pain, University of Kentucky College of Dentistry, Lexington, USA. 2Department of Anesthesia, University of Kentucky College of Medicine, Lexington, USA. 3Department of Psychology, University of Kentucky Arts and Science, Lexington, USA
Poster 26
Management of Nummular Headache using the CGRP Inhibitor Galcanezumab: A Case Report
Authors: Mitchell, A1 and Moreno-Hay, I1
Affiliation: 1University of Kentucky College of Dentistry, Department of Oral Health Science, Division of Orofacial Pain; Lexington, KY, USA
Poster 27
Treatment of Invasive Candida Osteomyelitis of the Jaw: A Case Report
Authors: Park, HJ1; Choi, HI2; Jeong, SR3; Ryu, JW1
Affiliations: 1Department of Oral Medicine, School of Dentistry, Chosun University, Gwangju 61452, Republic of Korea. 2Department of Oral and Maxillofacial Surgery, Chosun University Dental Hospital, Gwangju . 3 Chosun University 61452, Republic of Korea Department of Orthodontics, School of Dentistry, Gwangju 61452, Republic of Korea
Poster 28
Blast-Induced Orofacial Pain in a Rodent Combat and Operational Stress Model
Authors: Priess, MR1; Garza, TH1; Trevino, AV1; Szczesniak, A1; McCloskey, MP1; Greene, WA1; Clifford, JL1; VandeVord, PJ2; Stark, TR1; and Urban, MJ1
Affiliations: 1U.S. Army Institute of Surgical Research, JBSA Fort Sam Houston, TX. 2Center for Injury Biomechanics, Virginia Polytechnic Institute and State University, Blacksburg, VA
Poster 29
Use of Oral Devices in the Management of Oral Dysesthesia: A Case Series
Authors: Chirravur, P1,2,3; Vacharotayangul, P4, 5; Sroussi. H4,5; Klasser, GD6
Affiliations: 1Oral and Maxillofacial Diagnostic Sciences, UCONN Health, 2John Dempsey Hospital, 3Neag Comprehensive Cancer Center, Farmington. 4Division of Oral Medicine and Dentistry, Brigham, and Women’s Hospital, 5Department of Oral Medicine, Infection, and Immunity, Harvard School of Dental Medicine, Boston. 6Department of Diagnostic Sciences, Louisiana State University, School of Dentistry, New Orleans